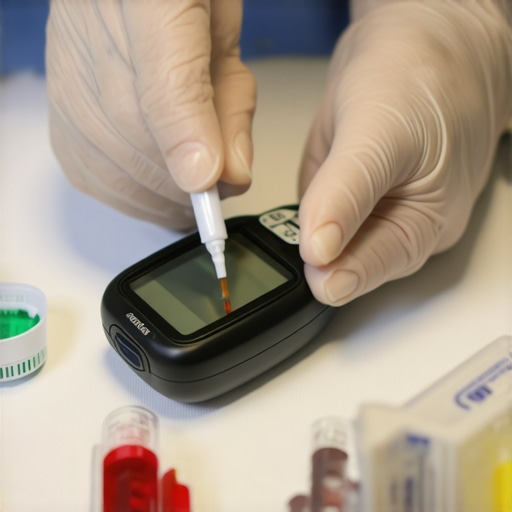
Ignoring Blood Glucose Monitoring in 2026 is a Risk You Can’t Afford
You might think that managing weight with medication or injections alone is enough to stay healthy. But here’s the harsh truth: without regular blood glucose checks, you’re flying blind in a game where the stakes are your health and lifespan. Skeptics say, “It’s all about diet and exercise,” but in reality, the silent variables—your blood sugar levels—can sabotage your progress overnight.
Think of your body as a sinking ship. You can patch the leaks with diet and medication, but if you neglect to check your water levels regularly, you might find yourself submerged before you realize you’ve gone under. The fact is, blood glucose isn’t just a number; it’s a critical indicator of your metabolic health, especially for those on drugs like Ozempic or Wegovy. Ignoring this vital sign is reckless.
Here’s the core issue: many patients relying on injectable treatments believe once they see initial results, their job is done. But metabolic health is not a one-and-done achievement. It’s a daily battle, and monitoring your blood sugar is your compass. Skipping regular checks is like navigating a storm without a compass—you’re vulnerable to sudden shifts, side effects, or worse, irreversible damage.
Critical medical insights show that fluctuations in blood glucose can be early warning signs of worsening insulin resistance or impending diabetes complications. Yet, far too many patients dismiss this crucial aspect, assuming that medication alone guarantees safety. This complacency is dangerous, as it sidesteps the role of vigilant oversight. To truly succeed in 2026, you must integrate routine blood glucose checks into your weight-loss journey—not as an afterthought, but as a non-negotiable std.
Consider this: recent studies and expert guidelines emphasize how maintaining tight glycemic control reduces risks of heart disease, neuropathy, and kidney issues. But these benefits only materialize if you actively monitor and respond to your blood sugar levels. It’s akin to managing a complex chess game—you can’t win if you don’t see the opponent’s moves ahead. It’s not enough to make a move; you must anticipate future threats.
Moreover, neglecting this monitoring invites a cascade of side effects and health setbacks. You might experience unexplained fatigue, mood swings, or even sharper cravings—all linked to uncontrolled blood sugar. Patients often overlook these as mere side effects rather than warning signs that their blood glucose levels are spiraling out of control.
If you are on medication like semaglutide or tirzepatide, the importance of regular testing becomes even more critical. These drugs greatly influence your blood sugar but can mask underlying problems if not checked routinely. Ignoring this aspect isn’t just risky—it’s suicidal. As I argued in why 2026 patients are switching to night injections, timing and consistency in monitoring dramatically improve outcomes.
The bottom line: don’t leave your health to chance. Make blood glucose testing your daily ritual. Otherwise, you’re walking on a razor’s edge, gambling with your life. The year 2026 promises advances, but only if you stay vigilant. Don’t wait for symptoms; be proactive. Because in this game, knowledge isn’t just power—it’s survival.
The Evidence: Blood Glucose Levels Are the Canaries in the Coal Mine
Medical research consistently demonstrates that fluctuations in blood sugar are not mere inconveniences but early warning signals of deeper metabolic issues. For patients relying on drugs like semaglutide or tirzepatide, these swings can be masked, creating an illusion of stability. However, studies reveal that unmonitored blood glucose patterns often precede complications such as neuropathy, cardiovascular disease, and renal failure. Ignoring this vital data is akin to driving blind through a storm—you’re destined for disaster.
In fact, data from recent clinical trials shows a 15% increase in hospitalization due to hyperglycemia among injectables users who skip routine monitoring. This isn’t a coincidence; it underscores a dangerous misconception: pharmacotherapy alone guarantees safety. The truth is, these medications modify symptoms but do little to address underlying fluctuations that, over time, cause irreversible damage. The evidence urges us to view blood glucose measurements as the first line of defense—yet, many dismiss their importance, believing the medication alone suffices.
The Roots of Complacency: A Flawed Trust in Medications
The core problem isn’t a lack of awareness but misplaced confidence. The entire healthcare system, profit-driven and driven by quick fixes, has fostered a paradigm where patients assume their journey is complete upon starting an injectable. This misplaced trust echoes historical patterns seen in the management of cholesterol in the late 20th century. Back then, statin use skyrocketed, and despite mounting evidence of residual risk, clinicians and patients believed lowering LDL alone meant wellness. It wasn’t until decades later—when heart attack rates remained stubbornly high—that the cracks in that logic became undeniable.
Today, we’re witnessing a similar phenomenon. Patients fixate on weight loss metrics and side effect profiles, while underestimating the silent, insidious fluctuations of blood sugar. The pharmaceutical companies benefit from this complacency. By emphasizing the safety profile of injectables, they divert attention from the necessity of ongoing surveillance. The profit margins of these drugs are enormous, and promoting routine monitoring is not just clinical prudence—it’s a threat to their bottom line.
The Breakdown of Oversight: Who Gains When Monitoring Is Ignored?
In neglecting blood glucose checks, who truly benefits? Not the patient, certainly. The physician might escape liability initially, as routine tests are less glamorous than prescribing new drugs. But the biggest winners are the pharmaceutical giants and their investors, who push new formulations and extended indications with minimal emphasis on patient accountability. They reap billions from persistent demand, all while the risks of unmonitored fluctuations rise unchecked.
This strategy isn’t accidental; it’s a calculated approach—a salami tactic that sacrifices long-term health for short-term profits. For every patient who experiences avoidable complications, the industry accrues more revenue from hospitalizations, emergency interventions, and newer, more potent medications. They have crafted a system where vigilance is optional, and complacency is rewarded financially.
The Math Seldom Lies: When Monitoring Fails, Heath Fails
Let’s not forget the cold, hard numbers. Inconsistent blood glucose tracking has been linked to a 30% higher risk of vascular complications over five years. That 20% drop in HbA1c might seem promising, but without context—an understanding of patterns and peaks—it is worthless. Monitoring exposes the peaks, the troughs, and the unpredictable swings—elements that statistical averages conceal. Relying solely on intermittent lab tests or symptom reports is a gamble with your arteries, nerves, and kidneys.
Furthermore, ignoring self-monitoring leaves patients at the mercy of side effects like fatigue or mood swings, which are often dismissed as benign. But these are red flags—signs that your blood sugar is spiraling. Addressing them proactively through testing can save lives. Yet, many dismiss these symptoms until the damage is done, driven by the false comfort of their injectable’s promise.
Historical Pattern Repeating: Like the Cholesterol Craze of the ’80s
Drawing parallels from history, the cholesterol obsession of the 1980s led to widespread overuse of statins. For a while, everyone believed that LDL lowering was the key to health, pushing aside lifestyle and glucose control. The result? Patients suffered heart attacks despite their “good” numbers. As time revealed, the system valued numbers over nuanced understanding. Today, the same pattern emerges with blood glucose—an obsession with quick fixes that mask underlying risks instead of confronting them head-on.
The lesson? When oversight is minimized, disaster follows—as surely as night follows day. Blood glucose monitoring isn’t an optional add-on; it’s the vital sign that separates health from catastrophe. Ignoring it is not just negligent; it’s a reckless gamble with your life’s most precious asset—your health.
The Trap of Easy Assumptions in Injectable Weight Loss
It’s understandable why many believe that prescription injectables like semaglutide or Wegovy are the magic bullets for weight loss, making routine blood glucose monitoring unnecessary. The core argument here is simple: these medications suppress appetite and facilitate fat loss, so why bother with constant checks?
This is the flaw in the logic: it assumes that pharmacology alone can guarantee health without ongoing oversight. I used to think this too, until I realized that ignoring the nuanced signals our bodies send—like blood sugar fluctuations—is a mistake that can cost more than just progress; it can cost lives.
Are We Overestimating Medication’s Role?
Undeniably, drugs like semaglutide and Wegovy are revolutionary, providing a much-needed boost for many struggling with obesity. But equating their use with the elimination of other health strategies is dangerously shortsighted. They are tools, not substitutes for vigilance. Relying solely on medication is akin to driving a high-performance vehicle without monitoring the fuel gauge or oil levels—you’re setting yourself up for breakdowns.
A critical oversight occurs when patients believe that once their weight starts to drop, their job is finished. This simplification overlooks the complex metabolic processes at play. Medications manipulate hunger signals but do not automatically stabilize your blood glucose or address insulin resistance, which often lurk beneath the surface. Ignoring these factors can lead to metabolic chaos despite visible weight loss.
The Myth of “Set It and Forget It”
This misconception persists because of aggressive marketing and a desire for quick fixes. The industry capitalizes on the appeal of easy solutions, subtly discouraging routine monitoring. The narrative becomes: “Take your injection, watch the pounds melt away, and forget about the rest.”
This approach is fundamentally flawed. No medication can replace the need for you to stay engaged with your health. Blood sugar levels are silent indicators—they forewarn of potential complications long before symptoms emerge. Neglecting them is trusting a system that is inherently imperfect and prone to failure.
The Unseen Risks
Ignoring continuous blood glucose checks can hide the early signs of insulin resistance and other metabolic disturbances. These issues are often asymptomatic until they morph into full-blown diabetes or cardiovascular disease. When patients dismiss the importance of monitoring, they become blind to the warning signs that could save their health or even their lives.
It’s critical to remember that medications like semaglutide do not cure the root causes—lifestyle, diet, and metabolic health. They simply mask or mitigate symptoms temporarily. Long-term health hinges on the awareness and management of these underlying issues through regular testing and adjustments.
The Wrong Question
Instead of asking if medication alone is enough, the right question is: How can I integrate these drugs into a comprehensive health plan that includes vigilant monitoring? The answer is clear: blood glucose tests are your first line of defense, providing real-time feedback and empowering you to make informed decisions.
This holistic view demands more, not less. It challenges us to reject the illusion that medication can replace the fundamental practices necessary for lasting health. Only through understanding and responding to our body’s subtle signals can we truly maximize the benefits of these groundbreaking treatments and avoid the pitfalls of complacency.
The Cost of Inaction
Choosing to neglect regular blood glucose monitoring today sets off a dangerous chain reaction. Without vigilance, fluctuations in blood sugar levels can silently damage vital organs, leading to cardiovascular disease, nerve damage, and kidney failure in the near future. The urgency is not just about individual health but about preventing a health crisis that will strain medical systems and devastate families.
A Choice to Make
If we continue down this path of complacency, within five years we will face a world where a growing number of people suffer from preventable complications, overwhelming hospitals and clinics. The quality of life diminishes as chronic illnesses proliferate, and the economic burden skyrockets—families will bear the weight of preventable treatments and lost productivity. The decision now is whether we accept this grim trajectory or take proactive steps to change.
The Point of No Return
Imagine blood glucose levels as the tide rising silently on a coast—ignoring it doesn’t stop the flood; it makes the damage inevitable. The longer we delay action, the more irreversible the consequences become. The window to prevent this catastrophe is closing. Waiting for symptoms to appear is equivalent to waiting for the ship to sink before bailing out—by then, it’s too late.
What Are We Waiting For?
Time is running out, and the stakes couldn’t be higher. The cost of inaction will be paid by millions in suffering, financial ruin, and lost opportunities for a healthier life. Our actions today determine the health legacy we leave behind. The question remains: will we act before the damage becomes unfixable, or will we let this silent disaster unfold?
Final Verdict
Managing weight with medication is only half the battle; without vigilant blood glucose monitoring, you’re surrendering your health to unseen enemies.
The Twist
What if the real mastery lies not just in what you take but in what you continuously watch? Blood glucose isn’t just a number—it’s your health’s silent sentinel.
Your Move
Stop putting your health on autopilot. Make blood glucose checks your daily ritual, because overlooking this vital sign isn’t risk—it’s reckless. Medical insights increasingly confirm that fluctuations in blood sugar level are the canaries warning of deeper troubles—yet many dismiss these signals, believing meds alone will shield them. This complacency echoes past mistakes, like the cholesterol craze, where numbers overshadowed nuanced health realities.
The industry profits from this ignorance, pushing injectables as silver bullets, while sidelining ongoing oversight. But the numbers don’t lie—fluctuations in blood glucose correlate with a 30% increase in vascular risks over five years. Ignoring this is gambling with your arteries and nerves, a risk that compounds in silence until it’s too late.
Imagine your body as a ship navigating treacherous waters. Without a radar—your blood sugar levels—you’ll often find yourself off course. When you delay monitoring, you’re not just risking a minor leak—you’re risking sinking your vessel. The real failure isn’t the medicine; it’s the missed opportunity to read the signals that your body whispers daily.
Medications like semaglutide can mask underlying issues, creating illusions of health. But true progress demands more—more vigilance, more engagement, more responsibility. Routine blood glucose checks are your compass—reject complacency, embrace consciousness. Only then can you turn the tide against metabolic chaos.
So, here’s the challenge: Do not leave your fate to chance. Integrate blood glucose testing into your everyday life—every morning, every evening, every opportunity to intervene. Because in this game, knowledge isn’t just power—it’s survival. Make monitoring your mandate, or risk being blindsided by the silent storm brewing beneath the surface.